DILLON, living with Duchenne.
About Duchenne
Duchenne 101
If you or your loved one have received or suspect a diagnosis of Duchenne muscular dystrophy, you may have many questions, including “What is Duchenne?”
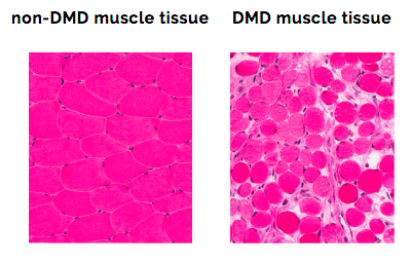
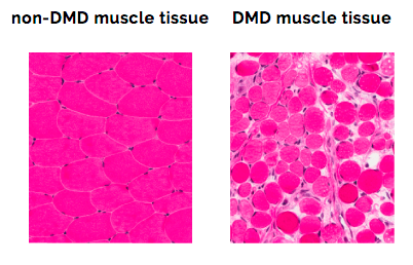
Duchenne muscular dystrophy is a rare, genetic condition that is characterized by progressive muscle damage and weakness.
Sometimes shortened to DMD or Duchenne, this rare disease is caused by a genetic mutation that prevents the body from producing a protein called dystrophin. Dystrophin acts like a shock absorber when muscles contract. Without dystrophin, muscles become more and more damaged and weakened. They may also lose the ability to repair themselves after an injury. Over time, children with Duchenne will develop problems walking and breathing, and eventually, the heart and the muscles that help them breathe will stop working. Duchenne is an irreversible, progressive disease. While there have been many advancements in the management of Duchenne, there is no cure at present.
Duchenne primarily affects males, with 1 in 3,500 to 5,000 boys born worldwide having Duchenne. In rare cases, it can also affect females.
Importance of Dystrophin
The dystrophin protein is needed for muscles to function properly. It is missing or found in very small amounts in people with Duchenne. Watch Jackie and John talk about the importance of dystrophin.
What Are Proteins?
Proteins are large, complex molecules that serve as the building blocks for almost all of the tissues and organs in the body and are essential for our bodies to function. Each protein has a specific job—for instance, helping you digest food, helping your hair and nails grow, or helping you fight off infection. To make proteins, the body needs instructions so it knows which ones to make and how to make them. These instructions are found in sections of our DNA called genes.
What Is Dystrophin?
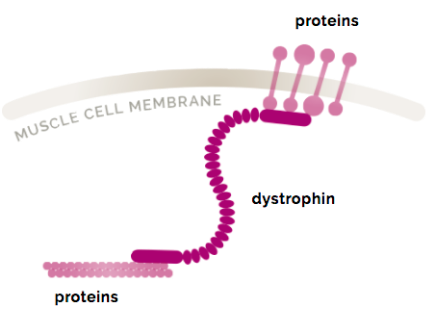
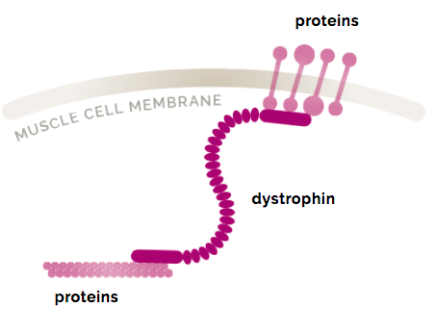
Dystrophin is a protein found in muscle cells. It is one of a group of proteins that work together to strengthen muscle fibers and protect them from injury as muscles contract and relax. Although dystrophin exists in small amounts in the body (0.002% of total muscle protein), it plays a vital role. Within a muscle cell, dystrophin has a very important job. It connects the cell’s inner support structure, or cytoskeleton, to the outside “skin” of the cell, also known as the muscle cell membrane. There, it acts like a trampoline spring, protecting the muscle cell from the damage caused by the normal wear and tear of muscle contraction. In Duchenne, the lack of dystrophin protein leads to a cycle of muscle cell degeneration, inflammation, and fibrosis, which damages skeletal, lung, and heart muscle tissue.
What Happens in Duchenne?
Duchenne is caused by errors in the dystrophin gene that lead to little or no dystrophin being produced. Most commonly, one or more exons (a portion of the gene) are missing, and the remaining exons do not fit together properly. Because of this error in the genetic instructions, cells cannot make dystrophin. Without dystrophin, muscle cells are damaged and over time are replaced with scar tissue and fat in a process called fibrosis.
Why Dystrophin matters
People living with Duchenne need functional Dystrophin, regardless of where they are in their journey. A lack of functional dystrophin can lead to continuous, irreversible muscle loss.
As early as age 2 to 5 years, changes to the heart have been observed
As early as age 5, respiratory changes have been shown to occur
A Little Dystrophin Can Mean a Lot
- When the body produces even small amounts of dystrophin, it can make a big difference
- Small amounts of dystrophin have been associated with longer ambulation, heart and lung function, and even survival compared to no dystrophin, based on observations of individuals with DMD in natural history studies
How Do We Know If Dystrophin Is Being Made?
There are now several ways we can measure the amount of dystrophin in muscle tissue. In clinical trials, doctors can take a sample of muscle cells during a test called a muscle biopsy. Then they do a series of very sensitive tests that look at the amount of dystrophin being produced and whether the dystrophin is located in the right area of the cell to do its job.
These tests are called:
Immunohistochemistry
- Using a powerful microscope and special dyes, researchers can see the location of the dystrophin and whether it is getting to the right part of the cell
Western blot
- A sensitive technique used in clinical trials to measure how much dystrophin is produced in muscle fibers
- Test samples are compared to a group of reference samples, called a standard curve, that have a known amount of dystrophin to determine the amount in each test sample
- Results can be affected by many different factors
- -How the samples are processed
- -The techniques to analyze them
- -The makeup of the standard curve
- -Methods of evaluating results
To address this, many companies work with the FDA to ensure their Western Blot method is acceptable.
Disease Progression
Duchenne muscular dystrophy weakens the body’s muscles over time.
And once muscle tissue is lost, it cannot be "fixed," which is why Duchenne is considered irreversible. However, some treatment options for Duchenne can help to slow disease progression.
In the early stages of Duchenne, the disease primarily affects the muscles of the hips and thighs. This can lead to difficulty standing, climbing stairs, and maintaining balance.
As the disease progresses, it affects the muscles in the shoulders and arms, leading to difficulties such as raising the arms. Additional muscles in the legs and trunk are also affected, as are the muscles that make it possible for you to breathe and for your heart to function. The rate of progression varies from child to child and is based on a variety of factors. Speak with your doctor to better understand what to expect for your child.
Independence and the Journey to Adulthood
Meet Tristan and Kenan, two young adult men living with Duchenne. Watch their videos to better understand their unique perspectives on independence.
Duchenne by Age Range
Below are descriptions of the clinical and muscle signs that may occur at various ages. Note that Duchenne progression varies greatly from person to person. The age ranges shown are approximate and each child may progress differently.
0 to 4 years
• Inflammation soon after birth
• Muscle fibrosis (scarring) seen as early as 1-year-old
• Motor delays
• Other delays, eg, speech
5 to 7 years
- Progressive muscle weakness
- Enlarged calves
- Toe walking
- Standing-from-supine difficulty
- Fat accumulation in muscle
The importance of age 7
- Natural growth stabilizes
- Disease starts to outpace functional gains
8 to 11 years
- Motor milestone delays
- Decreased walking ability
- Part-time wheelchair use
12 to 19 years
- Reduced upper limb, lung, and heart function
- Loss of ambulation
- Ventilatory support often required
- Unable to perform activities of daily living
Teens and Beyond
- Increasing heart problem
- Heart failure
- Life expectancy severely reduced